by Jackson Ambole Okata @amboleokata
This story was originally published in the Mt Kenya Times on September 30th
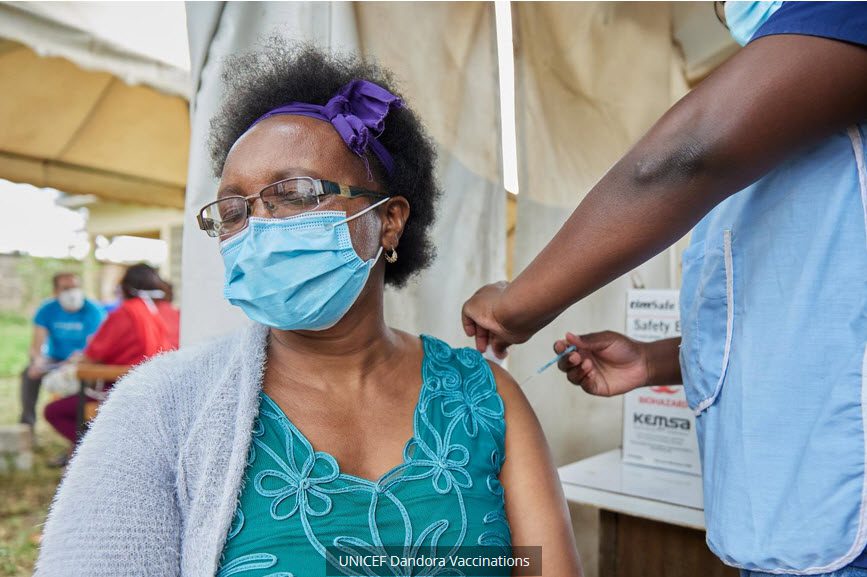
For 34-year-old Domitila Anyango getting the COVID-19 vaccine has remained a mirage, almost one year after she successfully battled the disease which she contracted while attending her uncle’s funeral in Siaya. The mother of two has been living with HIV for the past 14 years.
“I almost saw death for the six weeks I battled the virus at a Kisumu hospital. My support group came through and I was able to get the necessary care, though the coronavirus weakened my body to the core,” she told Mt Kenya times.
For months now, Domitila just like many of her colleagues living with HIV/AIDS has been trying to access the COVID-19 vaccine with no success. She has visited five vaccination centres with no success.
”The queues are long, and I cannot put up with that. On several occasions I have visited the vaccination centre only to be told that they have run out of the vaccine,” she said.
Challenges
Just like many African countries, Kenya is in a rush to get her entire adult population inoculated with the COVID-19 vaccine as a preventive measure against the coronavirus which almost brought the globe to a standstill.
And like many nations across the globe, Kenya is facing several challenges in her quest to get her people to receive the all-important jab. Limited vaccine availability, access and vaccine hesitancy are some of the issues the country must confront in its quest to achieve a fully vaccinated and protected population.
According to acting Director General of health Dr Patrick Amoth, Kenya targets to have vaccinated at least 10 million people of its 27 million adult population by December 2021.
Left Out
The country has made strides in the vaccination drive with frontline workers and groups of people being given priority. Healthcare workers, security personnel, teachers, hospitality industry workers and public transport workers were among the first groups of people to receive the jabs. Elderly persons were also included in the priority groups at a later stage.
But with all the efforts, the Ministry of Health seems to have omitted a critical group of people from those being prioritised for the vaccine.
Persons living with HIV/AIDS are being forced to encounter the struggles of getting the COVID-19 vaccine just like any other persons not under the priority groups.
According to data from the National AIDS Control Council (NACC), Kenya had a total of 1,388,169 adults living with HIV/AIDS as of 2019, many of whom are yet to be vaccinated.
NACC Chief Executive Officer Dr Masha Ruth says that currently the council does not have the actual number of persons living with HIV/AIDS who have been inoculated.
”The council is in the process of collecting data and tabulating. We want to establish how many persons living with HIV/AIDS have contracted the virus out of the total number of COVID-19 infections, how many died of the virus and how many have received the vaccine and that might take some time,” she told Mt Kenya times.
Hard to Find
Ernest Kibet, 48, a resident of Kipkelion in Kericho county is HIV positive and suffers from kidney failure and high blood pressure. He also contracted the coronavirus in February 2021. Kibet says that the experience was his worst in his entire life. ”I wouldn’t wish to see someone going through the pain I went through,” he says.
He says he was lucky to pull through after four months of hospital admission and he “saw the hand of God.” Kibet is among the lucky persons who have received the vaccine from the group of people living with HIV/AIDS. It took the intervention of a local human rights group in Kericho to have Kibet vaccinated.
The Afya vijijini lobby group stepped in after Kibet had severally turned away from vaccination centres.
Selina Chepkurui who led the push to get Kibet vaccinated says that the excuse of vaccine shortage could have seen him miss the all-important vaccine had they not stepped in.
”On several occasions he was turned away and told that he was not among the priority groups and when he kept on going, they told him that they had run out of vaccines and that is when we stepped in,” Chepkurui.
Chepkurui notes that it would have been prudent if the Ministry of Health included persons living with HIV/AIDS under the priority groups to receive the jab.
We are talking about people whose immunity is to some extent compromised, and it is wrong for the government not to classify them as a priority group.
Selina Chepkurui, HIV/Aids activist
“The government has all the data about persons living with HIV, and it’s upon them to roll out a mass vaccination exercise specifically for them just like they did for teachers and the police,” she said.
Hesitancy
National Taskforce on Vaccine Deployment Chairperson Dr Willis Akhwale, says that person living with HIV/AIDS are categorized under the group of persons living with underlying conditions who he says have been prioritized for vaccination. He however agrees that the group ought to be given special consideration because of their immunity status.
Dr Akhwale however dismisses the notion of vaccine shortage saying that the number of people vaccinated vis-à-vis the available doses is a clear indication that vaccines are available.
“We have over 4 million vaccine doses still available. People are simply not coming out to be vaccinated despite our persistent calls,” says Dr. Willis Akhwale
According to Dr Akhwale, the only solution to vaccine hesitancy will be a nationwide massive vaccination drive.
The Burden
Anne Moraa, 45, and a HIV positive mother of two has been unable to resume her hotel business in Molo town, which closed down when the pandemic struck. She says that failure to get the vaccine has complicated her return-to-work plans.
”I cannot take the risk of going back to business without first getting the jab because I know how my immunity is,” said Moraa. No vaccine means no work for Moraa and this has forced her to depend on well-wishers for survival.
”If I get the vaccine I will go back to work because I know I will be safe. Currently, my children are out of school and my rent is in arrears.”
Some HIV positive persons have been unable to receive the jab because they are unable to make it to vaccination centres mostly located miles away from their homes.
56-year-old Anne Njeri, a resident of Nyamamithi in Subukia, Nakuru county needs at least Ksh 400 to be able to access the nearest health facility which is 30 kilometres from her home.
”I have not received the vaccine because the facility is far, and the road is bad. The boda-boda riders are charging so much money and for now I cannot afford,” said Njeri.
The Target
As of the 26th of September 2021, Kenya had received a total of 6.35 million COVID-19 vaccine doses and managed to administer a total of 3.62 million doses.
Of the vaccinated, 2.73 million had received the 1st dose while slightly over 888,000 had received the second dose. Kenya has so far vaccinated 3.3% of its adult population.
Since the first case was reported, Kenya has recorded a total of 248,4621 COVID-19 cases as of 26th sept with 240,235 recoveries and 5.202 fatalities being recorded. The country has so far carried out 2,534 000 tests.
Kenya has continually been receiving vaccines among them AstraZeneca, PFIZER, Moderna, Johnson and Johnson, from the COVAX facility and from friendly countries like US, India, France, UK, Greece and Belgium.
To enhance the COVID-19 vaccine uptake, the government has rolled out a mobile vaccination drive to target areas not covered by health facilities.
A mass vaccination exercise targeting prison staff and inmates has also been rolled out with a target of vaccinating at least 50,000 people within the country’s correctional facilities.